Introduction
Healthcare providers face significant challenges in managing legacy data, a byproduct of outdated systems, mergers, acquisitions, and transitions to modern electronic health record (EHR) systems. Legacy data comprising medical records, diagnostic reports, treatment histories, and more remains critical for patient care, compliance, and research. However, its management poses issues related to storage, security, accessibility, and interoperability, often straining organizational resources and increasing cybersecurity risks.
This article explores the key challenges of legacy data management and offers actionable solutions to help healthcare providers navigate this complex landscape effectively.
The Healthcare Legacy Data Dilemma
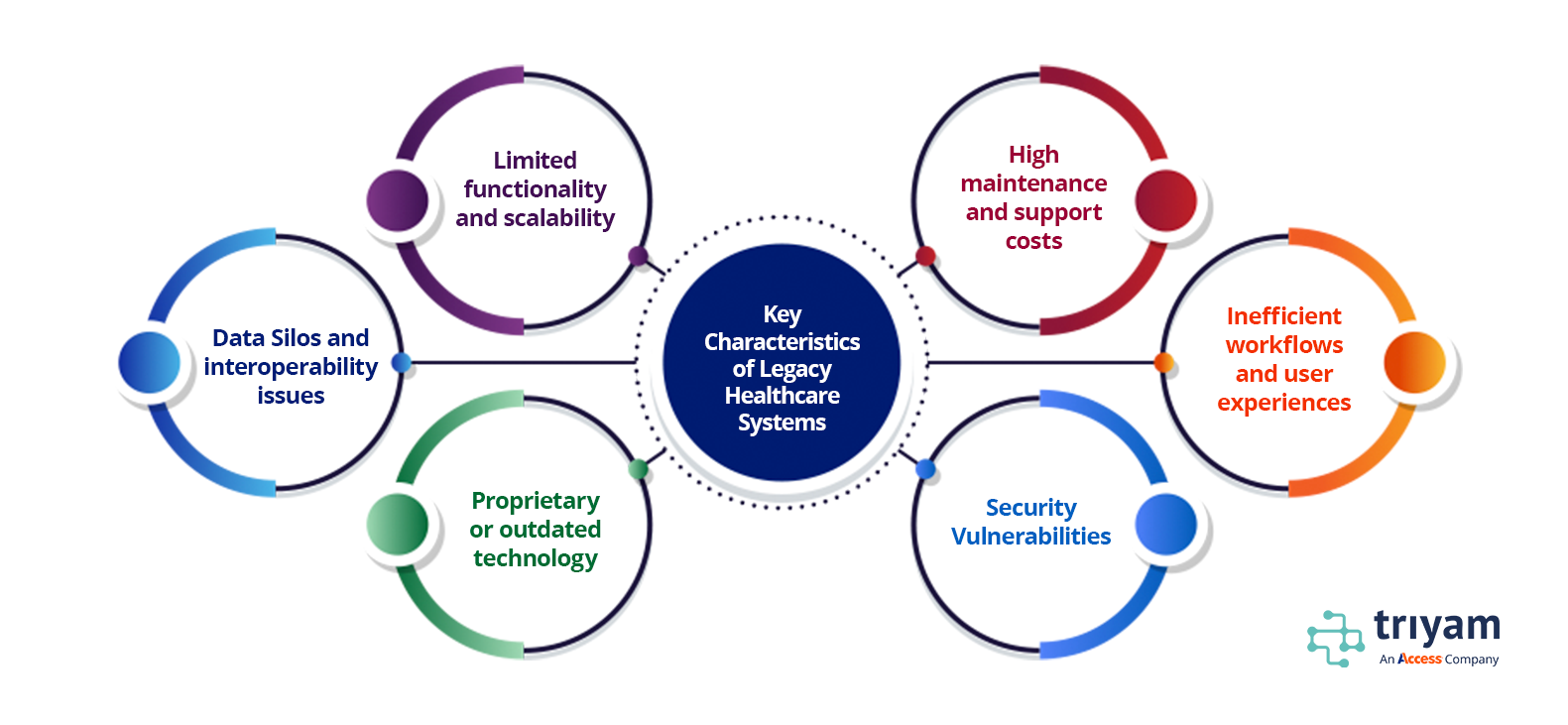
Legacy data accumulates as healthcare organizations evolve, often through mergers or upgrades to new EHR systems. According to a 2022 HIMSS survey, 73% of healthcare providers still rely on legacy systems, which are costly to maintain and prone to inefficiencies. These systems create data silos, hinder interoperability and pose security vulnerabilities due to outdated protocols. The following challenges highlight the complexity of managing legacy data:
-
- Storage and Cost- Legacy systems require ongoing maintenance, including server upkeep and software licenses, which can be a significant financial burden. For instance, a decade-old system with 300,000 lines of code can accrue over $1 million in technical debt, as noted in a Software Intelligence report. Retaining accessible legacy data for compliance purposes further escalates storage costs.
- Security Risks- Healthcare is a prime target for cyberattacks, with legacy systems being the third-biggest cybersecurity challenge, according to industry reports. Outdated servers and software lack modern encryption and access controls, increasing the risk of data breaches. In the first half of 2025, over 29 million individuals were affected by healthcare data breaches, underscoring the urgency of securing legacy data.
- Accessibility and Interoperability- Clinical staff need seamless access to historical records for patient care, while Health Information Management (HIM) teams require data for compliance and reporting. Legacy systems often lack integration with modern EHRs, creating barriers to data sharing. This can lead to delayed care, redundant testing, or errors, impacting patient outcomes.
- Data Quality and Governance- Legacy data is often fragmented and stored in varied formats across multiple systems, leading to inaccuracies and duplication. Manual data quality control processes, as noted in interviews with state health agency staff, are inefficient and error-prone, burdening IT teams and complicating compliance with regulations like HIPAA.
Solutions for Managing Healthcare Legacy Data
To address these challenges, healthcare providers can adopt a strategic, multi-faceted approach to modernize data management while ensuring compliance, security, and operational efficiency. Below are key solutions:
-
- Establish a Cross-Functional Data Governance Team
Creating a data governance team with an executive sponsor is critical for effective decision-making. This team should inventory all applications and data across the organization, documenting details such as data types, storage locations, and access requirements. A clear governance framework ensures compliance with regulations like HIPAA and GDPR (General Data Protection Regulation) while prioritizing data accessibility for clinical and operational needs.
-
- Modernize Legacy Systems
Modernizing legacy systems involves either upgrading or replacing outdated infrastructure. Cloud-based software-as-a-service (SaaS) solutions are increasingly viable, as they shift maintenance burdens to vendors and improve scalability. For example, cloud platforms with built-in interoperability features can bridge legacy systems with modern EHRs, enhancing data access. However, modernization must be carefully planned to avoid disruptions, as evidenced by past failed projects that resulted in resource losses.
-
- Implement Interoperability Solutions
Interoperability is key to unlocking the value of legacy data. Solutions like Single Sign-On (SSO) integrations, Master Patient Index (MPI) synchronization, and API-based connections can link legacy archives to modern systems. For instance, integrating an archive with patient portal streamlines record release workflows, and improving patient access. Adopting standards like HL7/FHIR ensures seamless data exchange across platforms, reducing silos and enhancing care delivery.
-
- Enhance Data Security
To mitigate cybersecurity risks, healthcare providers should invest in advanced technologies like encryption, blockchain, and AI-driven breach detection. Blockchain offers decentralized, tamper-proof data management, while AI can identify vulnerabilities in real time. Regular security audits and updates to legacy systems are essential to comply with regulations and protect sensitive patient data.
-
- Improve Data Quality and Cleaning
Data cleaning is vital to ensure legacy data is accurate and usable. Providers should implement automated data audits to identify and correct errors, reducing duplicates and inconsistencies. Clinical documentation improvement programs can train staff to capture high-quality data, supporting downstream analytics and decision-making.
-
- Leverage Point of Care (POC) Solutions
POC software enables real-time access to patient data, improving clinical decision-making and reducing paperwork. These HIPAA-compliant, web-based platforms can integrate with legacy systems, providing secure, encrypted access to historical records. By 2025, the POC data management market is projected to reach $11.7 billion, reflecting its growing role in enhancing efficiency and patient care.
-
- Partner with Experienced Vendors
Collaborating with healthcare IT vendors, such as those specializing in data migration and system integration, can streamline modernization efforts. Vendors can provide expertise in planning, staff training, and phased transitions, minimizing downtime and ensuring data integrity.
Benefits of Addressing the Healthcare Legacy Data Challenge
By implementing these solutions, healthcare providers can achieve several benefits:
-
- Improved Patient Care: Seamless access to historical data supports better clinical decisions, reducing errors and redundant testing.
- Cost Savings: Modernized systems and automated processes to lower maintenance and operational costs.
- Enhanced Security: Advanced technologies protect against breaches, ensuring compliance and patient trust.
- Operational Efficiency: Interoperable systems and clean data streamline workflows, freeing up resources for patient-focused activities.
- Data-Driven Insights: High-quality, accessible data enables analytics for research, population health management, and strategic planning.
Conclusion
The legacy data challenge is a critical issue for healthcare providers, driven by the complexities of outdated systems, security risks, and interoperability barriers. By establishing robust governance, modernizing infrastructure, enhancing security, and leveraging POC solutions, providers can transform legacy data into valuable assets. These strategies not only ensure compliance and protect patient information but also improve care delivery and operational efficiency. As the healthcare landscape evolves, proactive management of legacy data will position providers to thrive in a data-driven future.
Fovea EHR Archive addresses the healthcare legacy data challenge by enabling secure, efficient, and compliant data management. By leveraging AI-driven processes and cloud-based archiving, Triyam streamlines data migration, reduces maintenance costs, and ensures HIPAA compliance, allowing healthcare providers to decommission outdated systems while maintaining access to critical patient data. This approach enhances operational efficiency, improves patient care through seamless data accessibility, and supports long-term compliance with regulatory requirements, empowering healthcare organizations to focus on delivering high-quality care.